Putting Equity at the Center of Childhood Injury Prevention
Children in the U.S. die from injury at drastically unequal rates, with children who identify as Black, indigenous, rural, and/or lower income at highest risk. Identifying solutions to systematically address these inequities is paramount in making sure all children can access their human rights of health and safety.
An Update to the Nation’s First Pediatric Injury Equity Review
In 2022, we established the Massachusetts Pediatric Injury Equity Review (MassPIER) – a new process for reviewing inequities in injuries and identifying recommendations with experts in injury surveillance, child fatality review and legislative advocacy. Now, we are proud to share an update to this process to help hospitals across the country ensure more equitable care for children.
Partners:
- The Boston Medical Center (BMC) Department of Pediatrics (Project Lead)
- Johns Hopkins Center for Injury Research and Policy (Evaluation Partner)
- Massachusetts Department of Public Health (Data Collaborator)
- Suffolk, Middlesex, & Norfolk County District Attorney’s Office Child Fatality Review Teams (Collaborator)
A Framework for Understanding the Cause of Inequities
While injury prevention strategies have improved over the last decade and the prevalence of many injuries has decreased, inequities have persisted. Our team developed the Injury Equity Framework to better understand and address the complex factors which combine to worsen inequities in serious injuries.
This project, supported by the Bloomberg American Health Initiative, builds off an effective, data-informed process built on the Injury Equity Framework. The project was developed in 2021 and has helped Child Fatality Review teams and other public health focused groups identify drivers of childhood injury and develop meaningful recommendations. This enhanced model provides practical, easy-to-use tools that can be used to identify and address factors that impact the health and safety of children in their communities. The updated model and tools are described in depth in the accompanying toolkit, available for download.

The Injury Equity Framework provides a conceptual foundation to understand the complex multilevel factors which contribute to injury inequities. The framework is grounded in societal factors through which discrimination and stigma have operated historically and continue to operate today. These factors include ableism, classism, racism, sexism, homophobia, transphobia, and xenophobia, all of which operate at structural and individual levels. We'll review components of the framework, starting with intersectionality on the left. Intersectionality refers to the complex social identities which distinguish an individual or group, and include community, family, and individual factors. The intersectionality of an individual or group, within the context of societal factors, puts some individuals and/or groups at higher risk for an injury to occur, and for increased injury severity or and/or death.
The phases of injury are based on the Haddon Matrix, which is regularly used to describe factors that impact injury outcomes, and five major injury countermeasures distributed among the phases where they are most active. We created the Injury Equity Matrix as a companion working tool to the Injury Equity Framework to help teams develop effective interventions to better address injury inequities (available in the downloadable toolkit).
A Process Built on Real-World Feedback
After launching the MassPIER project in Massachusetts in 2021, the team gathered interview and focus group responses from Child Death Review teams throughout the state and nation. Using feedback from the interviews and focus groups, the team adapted the process and expanded resources to support teams across the country in systematically assessing injury trends and generating actionable recommendations.
The Pediatric Injury Equity Review (PIER) process is a structured, flexible framework grounded in the Child Fatality Review model and informed by evidence‑based injury prevention principles. PIER equips multidisciplinary groups with tools to review data, understand root causes, and translate findings into meaningful action.
The PIER model is adaptable for use at local, regional, or state levels and can be applied beyond fatality review teams to any group aiming to reduce injury‑related harm and eliminate disparities. Through a lens that prioritizes equity, systems thinking, and collaboration, PIER guides teams from problem identification to actionable solutions.
The PIER process consists of three core steps:
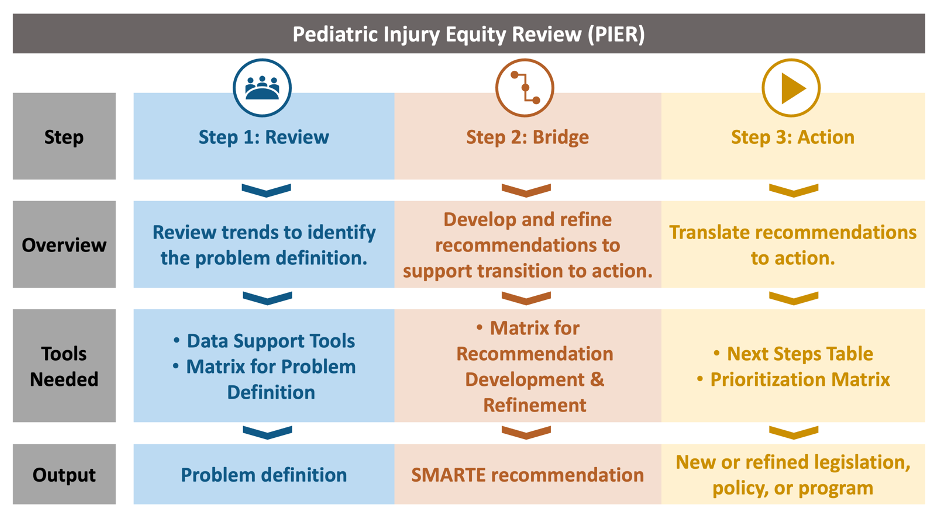
Step 1: Review
In Step 1, groups examine individual deaths or patterns of injury deaths in the context of population‑level injury data to understand patterns, inequities, and modifiable contributing factors. Using the PIER Matrix for Problem Definition, the group reviews systems-level modifiable contributing factors, discusses factors specific to their context, and develops a problem definition that will serve as the foundation for developing solutions in Step 2.
Step 2: Bridge
Step 2 focuses on transforming identified problems into actionable, population‑level recommendations. After reviewing and refining the problem definition, the PIER Matrix for Recommendation Development is used to develop recommendations across the domains of Built Environment, Equipment & Technology, Education, Treatment & Recovery, and Other factors. The recommendation is then refined to prioritize equity, to be SMARTE, and to support implementation planning.
Step 3: Action
Step 3 operationalizes the work completed in Steps 1 and 2, or can be utilized independently if recommendations have been previously developed. This step includes prioritizing recommendations using the PIER Prioritization Matrix, which supports decision making based on feasibility, impact, political will, community acceptance, evidence, and resources and capacity. After recommendations are prioritized, the PIER Next Steps Table is used to break each recommendation into clear, manageable action steps. The action step centers collaboration, shared ownership, and real‑world movement toward reducing pediatric injury disparities.
Save children’s lives in your community by implementing this process to identify solutions.
If you are ready to make a difference, take the first step today by downloading the tools you need. The PIER process is accessible to teams of all sizes and capacities. These three steps could make a world of difference for young people in your community.

- Complete Toolkit
- Matrix for Problem Definition Template
- Matrix for Problem Definition Library of Causes of Death
- Matrix for Recommendation Development & Refinement Template
- Prioritization Matrix Template
- Next Steps Table Template
- Potential Data Sources
- Guideline for Identifying ‘Action Team’ Members
- List of questions and prompts to promote systems focus
- Partnerships
Research Partners
This project was made possible through the generous support of the Bloomberg American Health Initiative, and through a multidisciplinary collaboration between multiple experts and organizations. Below is a list of individuals and groups who were instrumental in moving this work forward.
Principal Investigator, PIER
Chief Medical Officer, Safe Kids Worldwide
Associate Division Chief of Academic Affairs & Research
Division of Emergency Medicine, Children’s National Hospital
Associate Professor, GW School of Medicine & Health Sciences
Program Manager, PIER
Senior Research Associate, Safe Kids Worldwide
Advisor
Advisor
Advisor
Advisor
Advisor
Advisor
Injury Prevention Policy Coordinator
Epidemiologist, Injury Surveillance Program
Norfolk County District Attorney's Office
Norfolk County District Attorney's Office
Advisor
Want to learn more?
For questions, support, or to request virtual or in-person technical assistance with the PIER process, please contact our team. We are here to help groups at all stages—from initial data review to full implementation—advance equitable, evidence‑based injury prevention in their communities.

